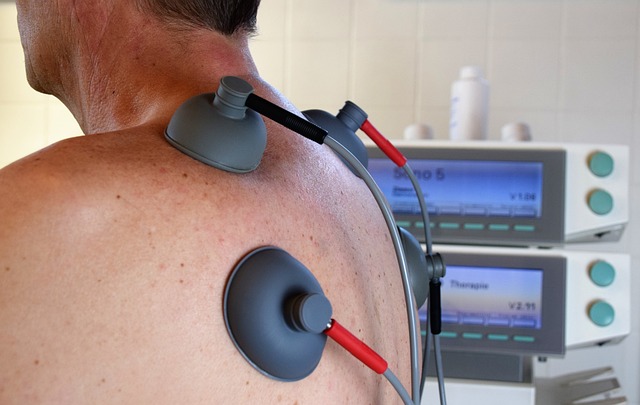
Running parallel to the pandemic has been the burnout epidemic afflicting those working in the healthcare sector. While the deluge of patients in need of care in the early stages of the crisis was undoubtedly a contributor, the bigger factor was the administrative responsibilities attached to that.
The Medscape National Physician Burnout & Suicide Report 2021 confirmed as much. Some 58 percent of the 12,000 physicians who responded to the survey listed the cause of burnout as being “too many bureaucratic tasks,” which was more than any other reason and consistent with the result of the 2016 poll. Just 16 percent of the respondents indicated that COVID-related issues like social distancing led to their stress, and just eight percent pointed to treating infected patients as the source.
In all, 42 percent of these physicians indicated they were burned out, though those in critical care (51 percent), rheumatology (50 percent), infectious diseases (49 percent) and urology (49 percent) trended even higher.
It appears that burnout is going to become a far greater issue in the years ahead, given the expected shortages of physicians and nurses. The doctor dearth could be as great as 139,000 by 2033, according to the Association of American Medical Colleges (AAMC), while the world’s nursing corps, which currently stands at 27 million, could be cut in half by 2030, according to the website DailyNurse.com.
That is coupled with the fact that the global population continues to age. The United Nations projects that there will be 1.5 billion people in the world over the age of 65 by 2050, more than twice as many as in 2019. In the U.S. alone the 65-and-over population is expected to approach 90 million by 2050; it stood at 46 million in 2019.
Obviously, then, clinicians are in need of new solutions to deal with an ever-worsening problem. Technology, and artificial intelligence in particular, offers one such solution, as indicated by the fact that 84 percent of American healthcare systems turned to AI (or indicated that it was in their plans to do so) in 2020, a year-over-year increase of 39 percent.
Within that trend is a pivot toward Voice AI, which besides lightening the load on clinicians enhances the patient experience – and, it is hoped, leads to the best possible outcomes. This trend is a big reason healthcare venture funding totalled a record $28.3 billion in 2021.
That momentum has continued into 2022. As noted by the website Pymnts.com, two AI and natural language processing (NLP) platforms, Mendel and Syllable, announced $40 million funding rounds in April – Mendel to hasten development of a platform called Resolve, which will enable clinical information to be consolidated, and Syllable to continue the evolution of its Patient Assistant, a call center and scheduling solution.
The year has also seen Anelto, a remote patient monitoring (RPM) provider, make improvements to its in-home teleconferencing console, RemoteCareLive, and the healthcare platform Suki afford clinicians easier access to electronic health records via verbal prompts.
Also of interest was the announcement in February by Nuance that it was acquiring a mobile AI assistant called Saykara, which is able to analyze doctor-patient conversations and detect anomalies that might elude the human ear.
The inescapable conclusion, then, is that AI has emerged as an especially promising antidote to the burnout epidemic, an epidemic that is only expected to increase in severity. Certainly further AI developments can be expected, and will no doubt be needed.