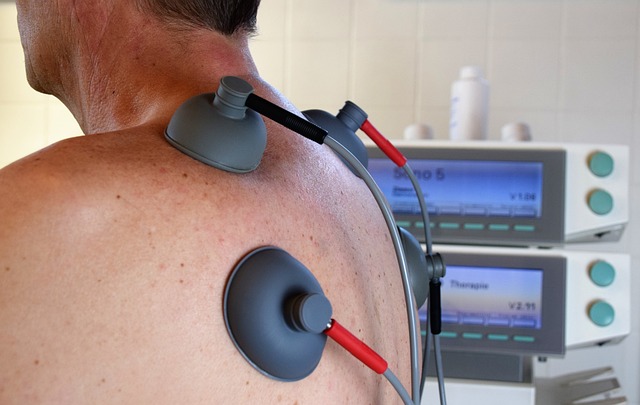
In April 2022, Dr. Helen Ouyang, a practicing physician, associate professor at Columbia University and New York Times contributor, examined in that media outlet virtual reality’s efficacy in managing chronic pain. In so doing she detailed the case of a retired high school biology teacher from Greenport, N.Y., named Robert Jester, who in 2016 broke his back in a fall off a ladder.
His pain grew so intense the first year after the accident that according to Ouyang he contemplated suicide. And while opioids helped alleviate his suffering to some degree, he did not like their impact on his personality, and was at a loss as to what other means of relief he might try.
He was introduced to VR through the father of one of the students he tutored, who reached out to a Los Angeles-based company called AppliedVR. That organization in turn supplied Jester with a headset, and his virtual visits to other travels – to a farm or the Wright Brothers’ plane, to cite two examples mentioned by Ouyang – reduced his pain to the point that he was off opioids within two months.
Affordability and scalability remain obstacles, but certainly Jester’s case is a striking example of VR’s potential in dealing with chronic pain, which is defined as pain lasting three months or more. It is estimated that at least 50 million Americans (and perhaps as many as 100 million) are afflicted with such pain, and managing it has been a major contributor to the opioid crisis.
It is estimated that eight of every 10 heroin users started out misusing prescription drugs, and in 2019 50 million Americans died from opioid overdoses. In other words, two of every three substance overdose fatalities were due to opioids.
The response in the healthcare community, according to Ouyang’s piece in the Times, has been to prescribe fewer pain medications, meaning that in a sense we’re back at Square One: How can chronic pain be effectively managed without subjecting patients to the danger of opioid addiction?
Dr. Brennan Spiegel of Cedars-Sinai Medical Center in Los Angeles began examining VR as a pain-management tool in 2015, and subsequent studies showed promising results. In 2017, for example, he found that patients felt 24 percent less pain after using the technology.
As Spiegel told Ouyang, “That’s because people can’t live in two realities at once.” She further noted that in his book VRx: How Virtual Therapeutics Will Revolutionize Medicine, Spiegel wrote that VR has an “ability to compel a person’s brain and body to react to a different reality.”
Moreover, the positive effects, as Jester found, continue after a patient removes his or her headset.
In November 2021 the Food and Drug Administration approved EaseVRx (since renamed RelieVRx) as a pain-management tool. It was developed by AppliedVR, the same organization that came to Jester’s aid, and in trials had resulted in two of every three subjects showing a 30 percent reduction in pain. Nearly half saw a 50 percent reduction.
The conclusion would appear to be inescapable, then: VR can ease chronic pain. While there are hurdles to negotiate in terms of making this technology an affordable option for as many people as possible, the bottom line is that it works, and can at the same time serve as an alternative to potentially dangerous opioids.