It’s no understatement to say that telehealth has exploded in popularity over the last several months. Faced with the once-in-a-lifetime challenge of navigating a global pandemic, patients initially flocked to telehealth solution because it would allow them to access convenient, high-quality care without breaking social distancing or inadvertently stressing already-overburdened health care centers. According to recent research, 46 percent of consumers are now using telehealth — a significant leap from the 11 percent reported in 2019. Providers are now seeing anywhere from 50 to 175 times the patients that they saw via telehealth before COVID-19.
But now, eight months into the pandemic, it has become clear that digitally-facilitated healthcare isn’t a one-off trend or stopgap measure. The same McKinsey report projects that given recent usage trends, greater provider adoption, and the extension of telehealth beyond virtual urgent care, as much as $250 billion of current US healthcare spend could be virtualized.
“Today, telehealth is largely a matter of convenience—which in and of itself has great value in improving access and lowering costs,” Hill Ferguson, the CEO of Doctor on Demand, shared in an article for Fierce Healthcare. “But telehealth will prove, in the coming months and years, that it will deliver better primary care to larger numbers of patients—and do so more efficiently than our current brick-and-mortar system.”
As we look to 2021, we need to consider how the telehealth tools we have come to rely on over the last several months could stand to improve healthcare provision even after COVID-19 wanes.
One major area of opportunity appears to be home healthcare.
“[Telehealth] is shining a spotlight on the home health care industry, which has long balanced connected and in-person care but – faced with a shortage of providers and a growing surplus of patients – could use more of the former and less of the latter,” one reporter for mHealthIntelligence wrote in an article on the field’s potential.
For context: the term home healthcare encompasses a wide range of care services provided in a patient’s home. This care method is typically less expensive, more effective, and equally effective as any care a patient might receive in a hospital or skilled nursing facility (SNF).
Home healthcare is often used to provide post-operative wound care, facilitate patient and caregiver education, and facilitate routine services such as intravenous therapy, medication injections, and daily illness support. The underlying goal is to treat a patient’s illness in a way that allows them to regain their independence and be as self-sufficient as possible. Home healthcare’s facilitation of patient autonomy has attracted a fair amount of interest in recent years as patients veer away from patterns of long-term, institutionalized care.
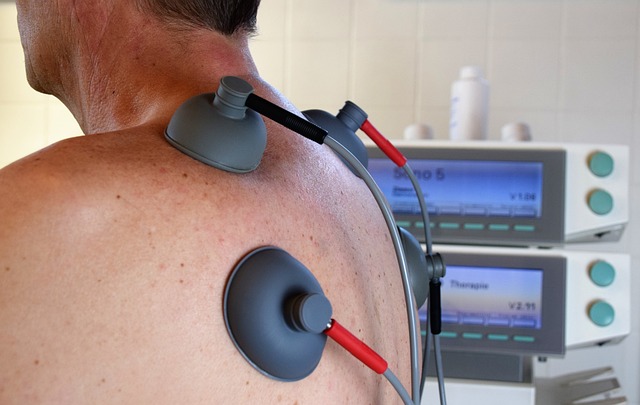
Telehealth appears to be in an excellent position to further the trend, too. In recent years, home healthcare providers have integrated digital remote monitoring and smart home products to allow patients to remain in their own environments — and out of care facilities — for longer.
“[Patients] want to stay home – that’s where they’re happy,” Mandy Johnson, the senior manager of the post-acute care coordination program at Banner Health, explained of home healthcare’s rising popularity in a recent article.
Johnson’s organization has made a point to act on this assessment; today, Banner Health presents a case study on how telehealth tools stand to augment and support existing home healthcare services. Over the last several years, Banner’s Home Healthcare Program has partnered with Health Recovery Solutions (HRS) to provide chronic care patients, as well as those who have been recently discharged and have a high risk of rehospitalization, with no-cost telehealth kits. These kits include several Bluetooth-enabled devices that allow physicians to monitor vital signs, collect critical health data, and determine how they might adjust a patient’s treatment plans to better support daily routines.
This digital support may be the key to expanding home healthcare in an era where people are more interested in — and savvy with — digital health technology. It’s also reasonable to assume that by increasing at-home services, providers may be able to significantly bolster patient outcomes, as past research indicates that elderly adults tend to recover faster and experience fewer complications when they receive home healthcare. At-home support also reduces the risk of falls, as patients are more familiar with their surroundings and can conduct their daily routines with confidence. Home healthcare further supports seniors’ independence, saves money, prevents avoidable hospital trips, and lessens the pressure on family caregivers.
The rationale for using telehealth to support and expand home healthcare services is clear — but there are barriers in place.
While digital health tools have been on the market for several years, the home healthcare sector has historically faced challenges in making their use of the technology financially-feasible. This is primarily due to a lack of support from the Centers of Medicare and Medicaid Services (CMS), which has limited reimbursement for telehealth services. While Medicare does permit some telehealth use for home healthcare services, those allowances are curtailed by strict guidelines on which providers are allowed to prescribe telehealth services and how many visits should be permitted.
All this said, some progress appears to be underway. Following the onset of COVID-19, CMS loosened its restrictions by permitting healthcare providers to apply telehealth tools as long as those services are part of the patient’s care plan and don’t replace in-person visits.
Given the potential benefits that telehealth stands to provide and the evident support that home healthcare offers to patients, we should advocate for an expansion of digital health solutions in the sector. Such a move would be beneficial for patients, payers, and providers alike — during and beyond the pandemic.